Blog articles filed under: General
Sleep Smarter, Live Better: World Sleep Day 2024
Posted March 15, 2024 by Brunswick Chiro / Category: General
Sleep Smarter, Live Better: World Sleep Day 2024
Posted Friday, Mar 15, 2024 by . Filed under General
We all know how important sleep is, yet many still underestimate the profound impact on our overall health and well-being it can have.
Are we getting enough sleep?
Sleep is essential to health
Sleep is a critical part of our health, like nutrition and physical activity. Benefits of sleep include:
- helps support memory and learning
- helps clear waste from the brain and promote brain health
- supports brain health, and brain health supports sleep
- supports immune health, and immune health supports sleep
- helps the immune system to clear bacteria and viruses
- helps to recycle old cells and maintain our bodies and energy levels

Sleepless Nights, Health Crisis
Let's look at sleep in another way, poor sleep health can have multiple significant impacts on human health:
Poor sleep as been linked to:
- obesity,
- diabetes
- coronary artery disease, and
- cardiovascular mortality
Poor sleep can lower immune response, creating greater susceptibility to infections that further reduce sleep quality.
Certain sleep disorders like obstructive sleep apnea and rapid eye movement sleep behaviour disorder are associated with:
- cognitive impairment,
- dementia,
- risk of seizures,
- and increased risk of stroke.
Poor sleep can result in reduced reaction times, impaired judgment, and cognitive impairment similar in effect to alcohol intoxication.
Drowsiness can impair safe driving even if the driver does not fall asleep.

Are You Achieving High-Quality Sleep?
One of the world sleep day organisations key messages this year is talking about "healthy sleep" and not just getting "enough sleep".
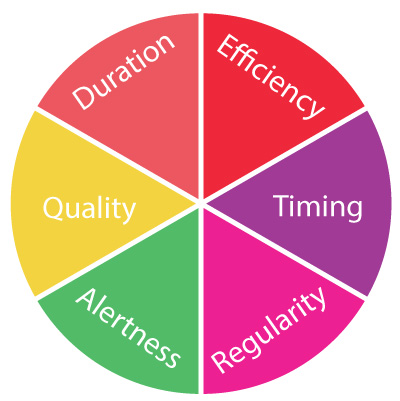
There are six dimensions that affect sleep health and consequently overall health and wellbeing:
- Duration: how much did you sleep over 24 hours
- Efficiency: how well do you fall asleep and stay asleep?
- Timing: when do you sleep?
- Regularity: do you have consistent sleep and wake times?
- Alertness: do you maintain good focus and attention during waking hours?
- Quality: do you feel satisfied with your sleep?
Our role in healthy sleeping
At Brunswick Chiropractic, we recognize the paramount importance of sleep in maintaining optimal health and well-being.
Our practitioners take a comprehensive approach to health and wellness, addressing both physical and lifestyle factors that can affect sleep.
Taking care of your aches and pains
Musculoskeletal disturbances can lead to discomfort and tension that may interfere with sleep. By correcting these issues, our practitioners aim to alleviate pain and promote relaxation, in order to facilitate better sleep.
Stress reduction
Our practitioners use multiple techniques (such as spinal manipulation and soft tissue therapy), which may help reduce stress levels. Chronic stress often contributes to sleep disturbances, so by addressing tension and promoting relaxation, we aid in calming the nervous system, making it easier to fall asleep and stay asleep.
Improving Sleep Posture
Poor sleep posture can strain muscles and exacerbate spinal misalignments, leading to discomfort and disrupted sleep.
We offer guidance on maintaining proper sleep posture and may recommend supportive pillows to promote spinal alignment and reduce pressure points, resulting in more restful sleep.
Lifestyle Advice
Our practitioners provide holistic guidance on lifestyle factors that impact sleep, such as diet, exercise, and stress management. They may offer recommendations for relaxation techniques, ergonomic adjustments, and sleep hygiene practices to optimize sleep quality and promote overall well-being.

Resources
https://worldsleepday.org
Cassidy S, Chau JY, Catt M, et al. Cross-sectional study of diet, physical activity, television viewing and sleep duration in 233,110 adults from the UK Biobank; the behavioural phenotype of cardiovascular disease and type 2 diabetes. BMJ Open 2016; 6: e010038
Hale L, Troxel W, Buysse DJ. Sleep Health: An Opportunity for Public Health to Address Health Equity. Annu Rev Public Health. 2020;41:81-99. doi:10.1146/annurev-publhealth-040119-094412
Reyes-Resina I, Samer S, Kreutz MR, et al. Molecular Mechanisms of Memory Consolidation That Operate During Sleep. Front Mol Neurosci 2021; 14: 767384. 2021/12/07. DOI: 10.3389/fnmol.2021.767384
Nedergaard M and Goldman SA. Glymphatic failure as a final common pathway to dementia. Science 2020; 370: 50-56. 2020/10/03. DOI: 10.1126/science.abb8739
Ju YE, Lucey BP and Holtzman DM. Sleep and Alzheimer disease pathology–a bidirectional relationship. Nat Rev Neurol 2014; 10: 115-119. 2013/12/25. DOI: 10.1038/nrneurol.2013.269
Haspel JA, Anafi R, Brown MK, et al. Perfect timing: circadian rhythms, sleep, and immunity – an NIH workshop summary. JCI Insight 2020; 5 2020/01/17. DOI: 10.1172/jci.insight.131487
Min S, Masanovic B, Bu T, et al. The Association Between Regular Physical Exercise, Sleep Patterns, Fasting, and Autophagy for Healthy Longevity and Well-Being: A Narrative Review. Front Psychol 2021; 12: 803421. 2021/12/21. DOI: 10.3389/fpsyg.2021.803421
Covassin N, Singh P and Somers VK. Keeping Up With the Clock: Circadian Disruption and Obesity Risk. Hypertension 2016; 68: 1081-1090. 2016/09/14. DOI: 10.1161/HYPERTENSIONAHA.116.06588
Itani O, Jike M, Watanabe N, et al. Short sleep duration and health outcomes: a systematic review, meta-analysis, and meta-regression. Sleep Med 2017; 32: 246-256. 2016/10/17. DOI: 10.1016/j.sleep.2016.08.006
Covassin N and Singh P. Sleep Duration and Cardiovascular Disease Risk: Epidemiologic and Experimental Evidence. Sleep Med Clin 2016; 11: 81-89. 2016/03/15. DOI: 10.1016/j.jsmc.2015.10.007
Lim AS, Kowgier M, Yu L, et al. Sleep Fragmentation and the Risk of Incident Alzheimer’s Disease and Cognitive Decline in Older Persons. Sleep 2013; 36: 1027-1032. 2013/07/03. DOI: 10.5665/sleep.2802
Wennberg AMV, Wu MN, Rosenberg PB, et al. Sleep Disturbance, Cognitive Decline, and Dementia: A Review. Semin Neurol 2017; 37: 395-406. 2017/08/25. DOI: 10.1055/s-0037-1604351
Bonilla-Jaime H, Zeleke H, Rojas A, et al. Sleep Disruption Worsens Seizures: Neuroinflammation as a Potential Mechanistic Link. Int J Mol Sci 2021; 22 2021/11/28. DOI: 10.3390/ijms222212531
Koo DL, Nam H, Thomas RJ, et al. Sleep Disturbances as a Risk Factor for Stroke. J Stroke 2018; 20: 12-32. 2018/02/07. DOI: 10.5853/jos.2017.02887
Williamson AM and Feyer AM. Moderate sleep deprivation produces impairments in cognitive and motor performance equivalent to legally prescribed levels of alcohol intoxication. Occup Environ Med 2000; 57: 649-655. 2000/09/13. DOI: 10.1136/oem.57.10.649
American Academy of Sleep Medicine Board of Directors, Watson NF, Morgenthaler T, et al. Confronting Drowsy Driving: The American Academy of Sleep Medicine Perspective. J Clin Sleep Med. 2015;11(11):1335-1336. Published 2015 Nov 15. doi:10.5664/jcsm.5200
Older Posts...

Back to Reality
Posted February 10, 2024 by Brunswick Chiropractic / Category: General
9 Tips to help you transition back into Work after the HolidaysAs early December rolls around, anticipation for the holiday season builds. Amidst the frenzy of shopping, work-related Christmas gatheri...
New Years Resolutions
Posted January 08, 2024 by Brunswick Chiropractic / Category: General
Blog / General New Years Resolutions Posted Monday, Jan 8, 2024 by . Filed under GeneralPsychology-Backed Tips for success in 2024As we embark on a new year, the tradition of setting New Year's reso...
Supporting Men's Health: Our Mission this Movember
Posted November 01, 2023 by Cloe Crowhurst / Category: General
Blog / General Supporting Men's Health: Our Mission this Movember Posted Wednesday, Nov 1, 2023 by . Filed under GeneralNovember in Australia brings not only the promise of warmer days but also the ...
World Mental Health Day 2023
Posted October 10, 2023 by Brunswick Chiropractic / Category: General
World Mental Health Day - October 10 2023 “Our minds, our rights"World Mental Health Day, observed on October 10th every year, is a global initiative led by the World Health Organization (WHO) to r...
What is myotherapy?
Posted September 07, 2023 by Brunswick Chiro / Category: General
Blog / General What is myotherapy? Posted Tuesday, Sep 29, 2023 by Brunswick Chiro. Filed under GeneralRemedial massage, osteopathy, and chiropractic care are well-known to many, but myotherapy rema...
Osteoarthritis: From Wear-and-Tear to Wellness
Posted August 31, 2023 by Brunswick Chiro / Category: General
Blog / General Osteoarthritis: From Wear-and-Tear to Wellness Posted Friday, Sep 8, 2023 by . Filed under GeneralOsteoarthritis, often referred to as "wear-and-tear" arthritis, is a prevalent joint ...
Crack the Code to a Healthier You
Posted August 15, 2023 by Brunswick Chiropractic / Category: General
Crack the Code to a Healthier YouIn today's fast-paced world, where stress, sedentary lifestyles, and poor posture have become the norm, taking proactive steps to prioritize our health has never been ...
Embrace Winter Wellness: 5 Tips to Stay Healthy in Brunswick
Posted June 02, 2023 by Brunswick Chiropractic / Category: General
Welcome to Brunswick Chiropractic, where your well-being is our top priority! As the winter months approach in Brunswick and the surrounding suburbs, it's essential to adapt our lifestyles for optima...
Bridget's Marathon
Posted December 01, 2022 by Bridget / Category: General
WHERE IT ALL BEGAN I recently travelled to Queenstown, New Zealand, to run my first marathon - why not right?! 4 years in the making trying to make it to New Zealand; A nasty burst appendix an...
What is the best sleeping position?
Posted August 18, 2022 by Brunswick Chiro / Category: General
Do you wake up in the morning with back pain? If so, you're not alone. Millions of people suffer from back pain every day. The good news is that there are some things you can do to help alleviate the ...
8 tips for keeping your health in check over the school holidays
Posted June 26, 2022 by Brunswick Chiropractic / Category: General
It's that time of year again where the kids are out of school and parents are trying to figure out how to keep them entertained. While this can be a fun time for the whole family, it's also important ...
Some naturopathic winter advice from Cameron Mack our resident naturopath
Posted June 05, 2020 by Brunswick Chiropractic / Category: General
During this season, especially with our “semi lock down” restrictions, we can all fall into the trap of comfort and winter eating, pizza, pasta, breads, mashed potato, rice, take away. All...
We treat kids!
Posted November 14, 2018 by Brunswick Chiropractic / Category: General
Yes, we treat kids! Using very gentle techniques, there are a number of conditions that chiropractic has been shown to be helpful with. Call 9388 1233 to find out more....
Happy 1 year anniversary Teghan
Posted November 12, 2018 by Brunswick Chiropractic / Category: General
Happy Anniversaty Teghan - working with us for a year already! Thanks for everything that you do, always with a big smile... and helping to train our newest team member on proper phone etiquette....
15 year Chiro reunion
Posted November 11, 2018 by David Cannon / Category: General
Last night Dr Dave caught up with old mates from his RMIT Chiro class at their 15 year reunion!...
Flooding on Sydney Road
Posted November 07, 2018 by Brunswick Chiropractic / Category: General
Lucky we had the day off yesterday - you would’ve needed a kayak to come for your treatments! Sydney Road Brunswick was flooded! Thankfully we didn’t sustain too much damage, so we&rs...
Royal Park AMT Bronze Tournament
Posted November 04, 2018 by Brunswick Chiropractic / Category: General
We are proud to be sponsoring the Royal Park AMT Bronze tournament at Royal Park Tennis Club. Finals are on Monday - get on down to see the best players in action!...
The Osteo Team
Posted November 03, 2018 by Alicia Cannon / Category: General
Last weekend we got our osteopathy team together for a bit of a technique workshop. Meet Laura, Alicia, Teghan & Josh! Bookings available online - www.brunswickchiro.com.au - or call 9388 12...
Happy Halloween from Brunswick Chiropractic
Posted October 31, 2018 by Brunswick Chiro / Category: General
Happy Halloween! Come and get your spine checked today! 9388 1233...